Fourteen weeks ahead of his due date, Naphtal was unexpectedly delivered on a rural farm on the edge of Kono District, Sierra Leone, miles away from any health facility. He and his mother, who was in dire condition after a complicated, unattended birth, were rushed by ambulance to Koidu Government Hospital, Kono’s only hospital. None of the family’s neighbors, who had scrambled to call for help, thought that Naphtal would survive: He weighed less than two pounds, and without intensive, specialized neonatal care—care that had never existed in the rural, impoverished district, even at the highest-level health facility—loss seemed certain.
But all was not lost. Mere weeks prior, Koidu Government Hospital (KGH), which Partners In Health supports, had started a new Special Care Baby Unit: a dedicated neonatal ward stocked with the specialized equipment clinicians long needed to adequately care for infants born prematurely or with complications at birth.
“Baby Naphtal was in bad condition when he arrived at the hospital,” said Dr. Napthal Nyirimanzi, lead pediatrician at KGH. “He had hypothermia, respiratory distress, low blood sugar, and no sucking reflex needed to eat. The prognosis was poor.”
Poor—but not definite.
“Without the Special Care Baby Unit, we were not able to save any premature baby weighing less than two pounds,” Nyirimanzi said. “But we believed with the new facility, we could save this child.”
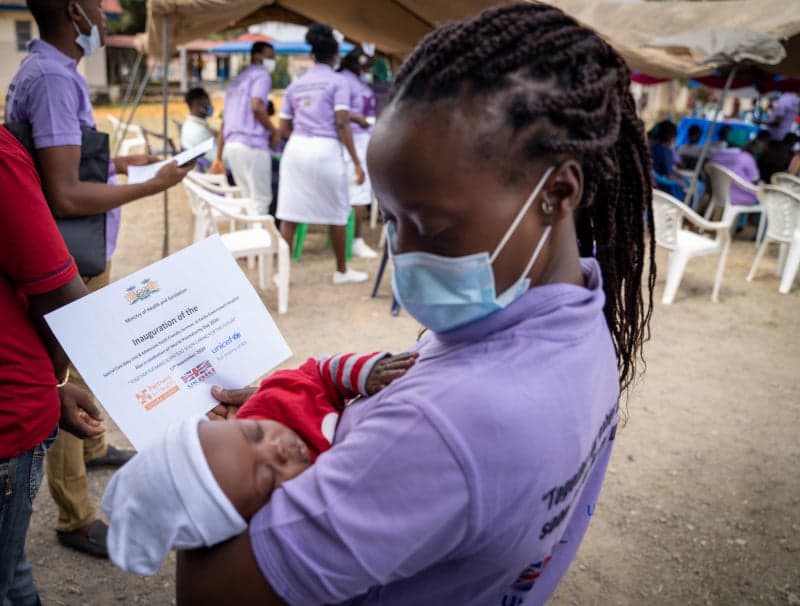
Opened in May by Sierra Leone’s Ministry of Health & Sanitation, in partnership with PIH and UNICEF, the Special Care Baby Unit provides care one level below that of a neonatal intensive care unit. Since opening its doors, the unit has already raised the quality of care for newborns at KGH and helped clinicians avoid worst case scenarios.
“A bad day for me—for most clinicians—is when I lose a patient I could have saved if I had the required equipment,” said Nyirimanzi.
Clinicians now have access to advanced medical supplies and equipment, from infant warmers and phototherapy lamps to vital sign monitors and emergency medications. And because the unit is attached to the maternity ward, they’re able to quickly transport newborns in need of emergency care. Those infants born at the hospital receive 24-hour care in a room separate from babies born outside of the hospital—a strict infection prevention and control system that keeps patients safe in their delicate states. And the unit also provides new clinicians with training and mentorship from pediatricians like Nyirimanzi, meaning more clinicians at KGH are developing crucial expertise in neonatal and pediatric care.
These new resources and protocols are tackling major barriers to saving at-risk infants. And they have helped keep newborns like Naphtal alive.
“Naphtal needed all the care extremely premature babies need to survive: oxygen support, infection prevention and control, antibiotics, temperature control,” Nyirimanzi said.
This vital care was available in the Special Care Baby Unit, allowing Naphtal to gain necessary weight and grow healthier.
Part and parcel with advancing care for vulnerable newborns, the Special Care Baby Unit prioritizes mothers as well. The unit provides an attached ward for mothers, allowing them to stay close to their babies round the clock without having to endure a long and costly commute between the hospital and home. During their stay, the women receive support with newborn care, including breastfeeding and “kangaroo care,” a lifesaving technique that emphasizes skin-to-skin contact between mother and newborn, which helps to naturally regulate the infant’s temperature and encourage feeding.
Kangaroo care was essential to Naphtal’s survival and growth—though it came not from his biological family, but from one of the caring nurses.
As is often the tragic, preventable case in Sierra Leone—a country with one of the world’s highest maternal mortality rates—Naphtal’s mother did not survive childbirth, largely due to chronic health conditions. His father was also in poor health and passed away soon after her death, leaving Naphtal orphaned by just one month old.
The parents barely met their son and did not live long enough to give him a name. Hospital staff searched for Naphtal’s relatives, but found no one able to adopt him due to the injustice of extreme poverty.
The hospital staff gave him a name: Naphtal, after Nyirimanzi, one of his primary caregivers and among the clinicians who had saved his life.
And another clinician emerged as a mother figure: Kadija Wurie Jalloh, a nurse in the unit.
After Naphtal’s birth, while clinicians desperately tried to save his mother, Jalloh provided kangaroo care to Naphtal, keeping him warm and helping him survive.
“His mother was so sick. I wanted her to see her baby okay,” said Jalloh. “Since she has passed, I said, ‘Let me take care of him.’ Because I don’t know who this baby will be in the future.”
Even on her days off from the hospital, Jalloh came to the Special Care Baby Unit and sat in the rocking chairs, holding Naphtal against her chest. She provided one of the blood transfusions that kept him alive. And she took him to receive his first vaccinations at the hospital’s under-5 clinic.
After five months in the Special Care Baby Unit, Jalloh took him home, vowing to care for him as her own unless a biological relative came forward.
“I love him so much,” she said.
Today, Naphtal is seven months old—small for his age, but healthy and continuing to grow.
“He’s the hospital’s baby,” Nyirimanzi said. “For me, baby Naphtal reminds me this: Commit yourself to save lives even whenever and wherever it seems impossible.”
Naphtal was among the first patients cared for at the Special Care Baby Unit—a symbol of impact to come. Since the unit’s opening, KGH has seen its neonatal mortality rate decline rapidly.
In September 2019, 13.8% of the hospital’s babies less than one month old died. By September 2020, just four months after the unit opened, that rate had dropped to 6.8%—a 51% reduction.
“Naphtal is a symbol that we can bring great change in what we do,” said Nyirimanzi. “That, even in resource limited settings, we can save lives.”
The Special Care Baby Unit’s opening comes as part of larger improvements to pediatric and maternal care at KGH. In late 2020, the hospital provided new trainings in pediatric emergency care and improved the monitoring of vital signs and medications, leading to a 65% drop in mortality in the pediatric ward. And PIH and the Ministry of Health have announced plans to build the Maternal Center of Excellence—an innovative, world-class maternal health center that will include a neonatal intensive care unit.
“The journey is long and we are still far from the ideal, but what matters is that we continue these steps toward improving maternal, neonatal, and child health,” Nyirimanzi said. “With the Special Care Baby Unit, we are on the right track.”
At home with Napthal, Jalloh looks forward to the hospital’s upward trajectory in caring for its tiniest patients.
“I’m proud of the work we’ve done,” she said. “We were losing babies. But now we are able to save so many.”